
Telemedicine Survey: Patient and Physician Adoption
Read Time: 0 Minutes
Telemedicine, as a concept, has been around since at least 1925, when Hugo Gernsback, a radio and publishing pioneer, predicted that physicians would use radio and TV to communicate with patients. In the February 1925 issue of Science and Invention, Gernsback wrote an article anticipating a device called the “teledactyl,” which would allow doctors to see their patients through a viewscreen and interact with them from a distance using the device’s robot arms.

Gernsback guessed that technology wouldn’t catch up to his teledactyl for at least 50 years, but rudimentary telemedicine technology began to appear in the late 1950s, when the University of Nebraska employed a kind of telemedicine that allowed it to send neurological exams and interact with patients. And by the end of the 1960s, the Nebraska Psychological Institute, working in conjunction with NASA, built telemedicine into a robust technology that could deliver real health care.
Early on physicians saw that telemedicine had the potential to reach patients in difficult geographies who lacked health care resources, but it wasn’t until about 2016 when it really entered the “mainstream.” In that year, the United States invested $16 million to improve health care in rural areas, dedicating part of the investment expressly to telemedicine.
Telemedicine Adoption
Up until recently, telemedicine has been slower to catch on. Elizabeth Bierbower, former Segment President of Employer Group and COO of Specialty Benefits, Humana, told us that, while both Medicaid and Medicare payers covered a patient’s telemedicine expenses, Medicaid’s support came with “significant restrictions,” a prime barrier to the true mainstreaming of telemedicine.
Simple awareness of telemedicine has also posed a problem. “Typically, when people have an issue, they want to call their doctor,” Bierbower said. “If their doctor doesn’t have [telemedicine], then their next thought is to go to the urgent care. Their natural impulse isn’t to call a telehealth provider.”
Further, provider adoption has proved challenging. Many physicians have not adopted telemedicine into their practice, and as Bierbower told us, “if [a patient’s] provider doesn’t offer [telemedicine], they may really be hesitant to go to a provider that they don’t know.”
But the pandemic is changing how the public, physicians, and payers look at telemedicine. “Up to now,” said Bierbower, “we’ve needed more awareness around this, and now the pandemic is bringing telehealth into the mainstream.”
Patients: Telemedicine Sentiment
GLG recently conducted a survey to take the temperature of the current landscape. We wanted to know how both patients and physicians regarded telemedicine. Was it a viable option? How did the two groups compare?
We asked a sample of 502 patients in the United States to rate what they thought about telemedicine for routine visits and follow-ups. The majority (55%) thought it was an “acceptable alternative to in-office visits,” while 26% regarded it as “preferable to in-office visits.” Only 19% regarded it as either a “poor” or “terrible” alternative.
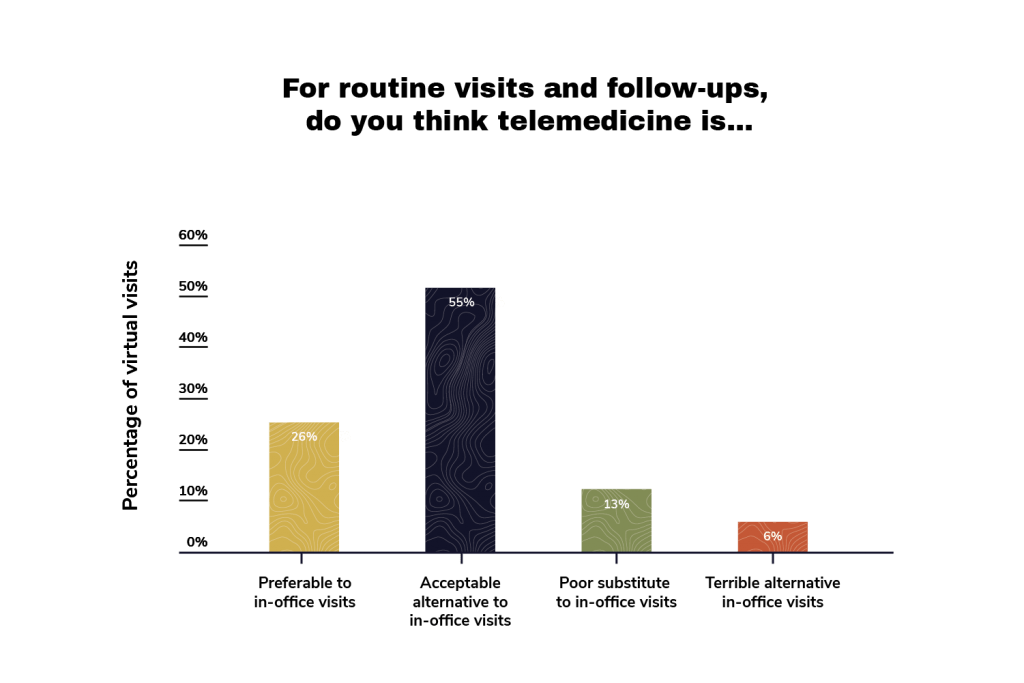
Physicians: Telemedicine Sentiment
GLG also surveyed 505 American doctors — a sample comprising 255 specialists and 250 primary care physicians — about how they believed their patients would rank telemedicine. The doctors largely agreed with the patients that telemedicine was an “acceptable” alternative, but diverged (10%) about whether it was “preferable” to an office visit. Instead, a quarter of those we surveyed (27%) said it was a poor substitute. Just 6% said it was a “terrible” alternative.
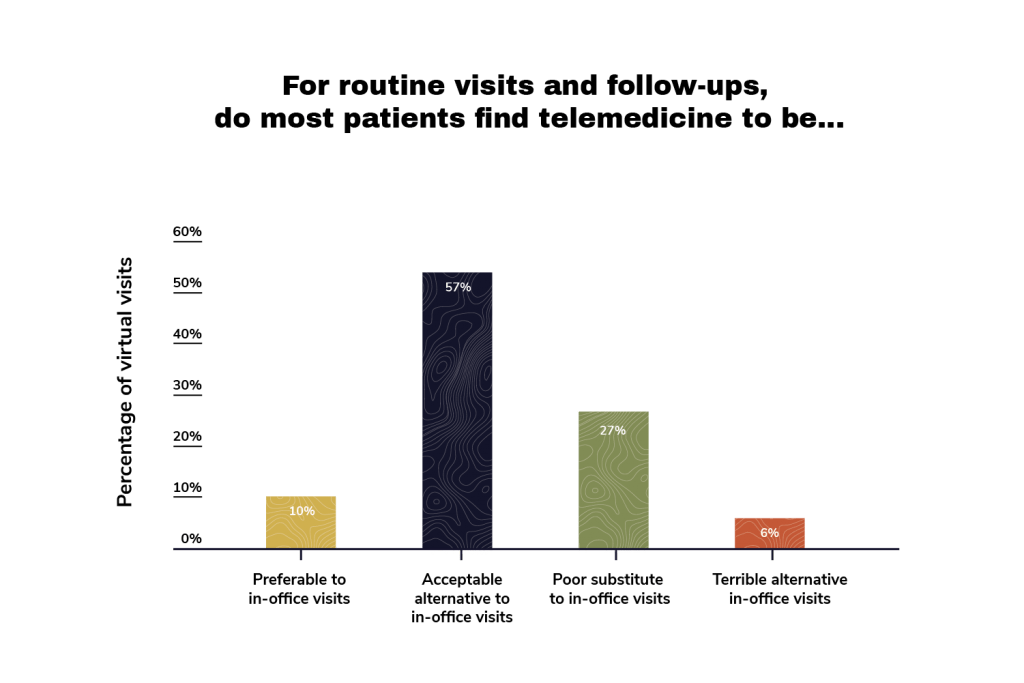
This changed when we broke the survey results between primary care physicians and specialists. Of the primary care doctors we surveyed, 74% of them said that they thought their patients would perceive telemedicine as “acceptable,” where only 41% of specialists said the same. The specialists in our survey also felt that telemedicine was a “poor” substitute to an in-office visit. Only 16% of primary care doctors felt the same.
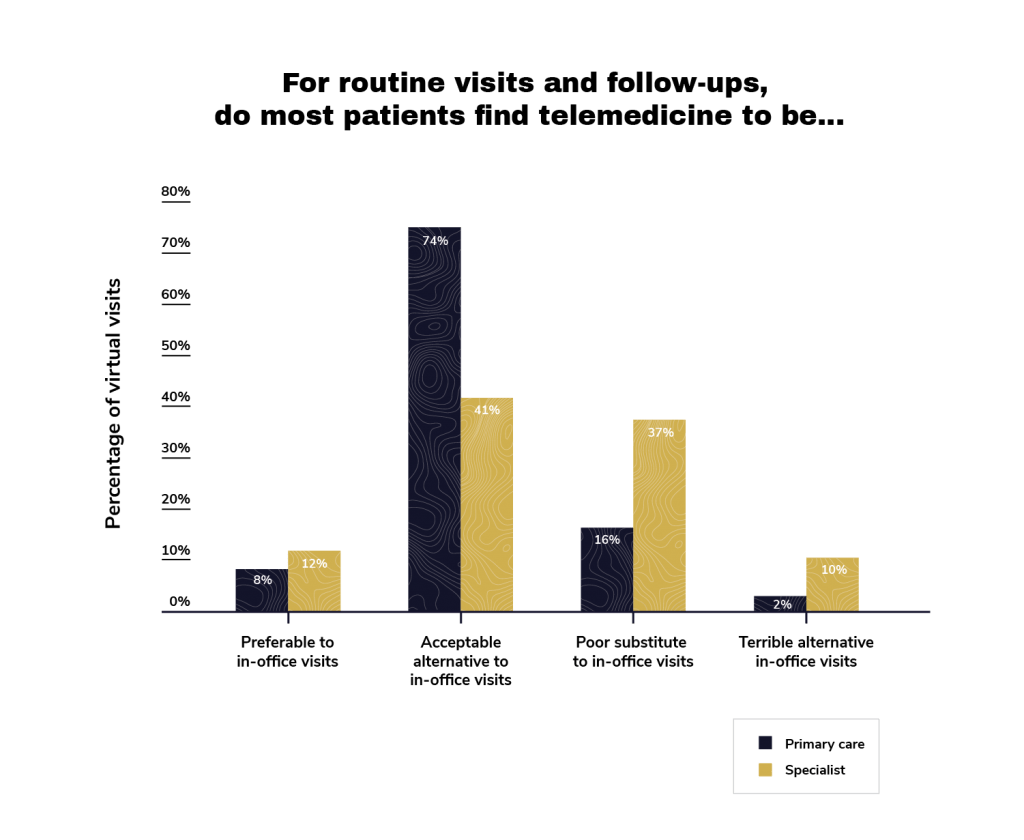
Telemedicine: Blip or Here to Stay?
GLG’s survey indicates that Bierbower was indeed correct in her assessment of telemedicine’s adoption. What’s interesting is that age of the practice is a factor in both its adoption and post-pandemic usage.
Anticipating telemedicine’s usage over time, 17% of the patients at the youngest practices (10 years or fewer) had already adopted the technology, while only 3% of those practices of more than 11-25 years and 4% of those of more than 26 years said the same.
Unsurprisingly, the pandemic drove telemedicine to surge in April, when lockdown orders were in effect, but the decline since has not returned it to pre-pandemic levels, and none of the physicians we surveyed think it will drop that far again. Demand will drop, but our survey indicates that telemedicine will have gained more mainstream acceptance.
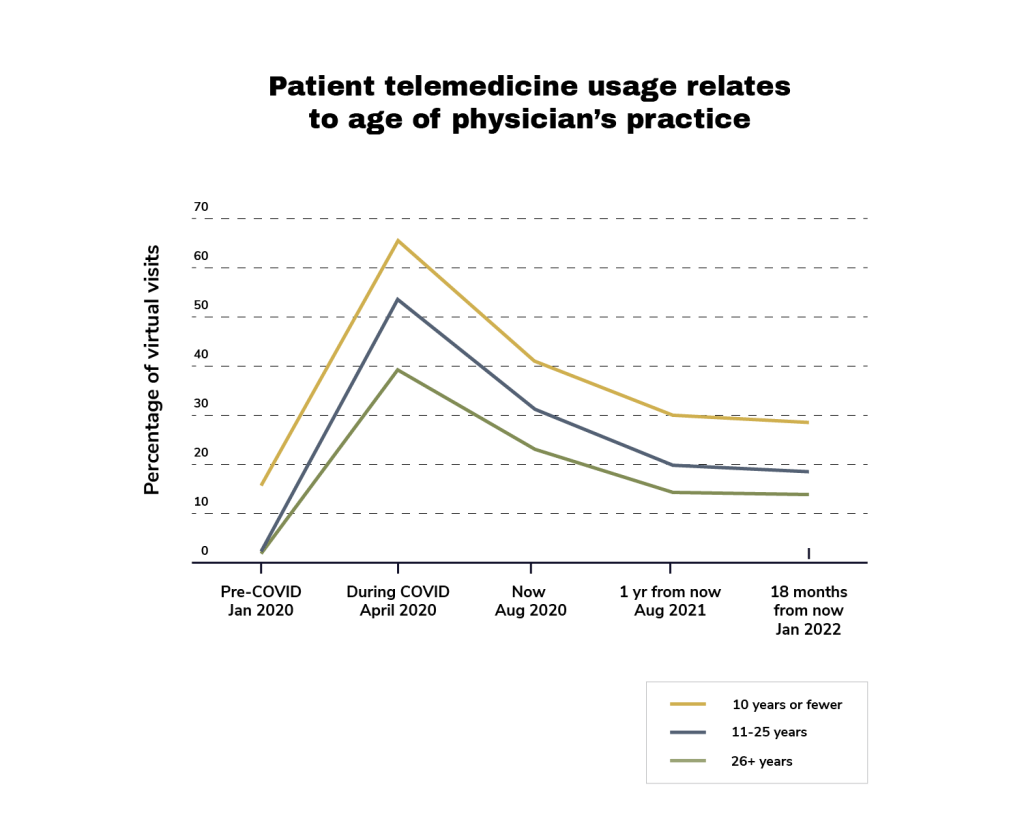
Telemedicine: The Regulatory Perspective
The surge that our survey shows in April could be a direct result of regulatory moves in March 2020. Sarah Lloyd-Stevenson, former Policy Adviser to the White House Domestic Policy Council and former Policy Adviser at the U.S. Department of Health and Human Services, told us that up until then, “the Social Security Act [was] very restrictive as to how telehealth services can be reimbursed in the Medicare program. With these [March] laws, HHS has been able to waive many Medicare restrictions and statutes across the country. This spurred the tidal wave of telehealth use that we’ve seen in the last few months.”
The question is whether Congress will act to make these waivers permanent. Lloyd-Stevenson told us that the waivers are something that she — and people like her — have been advocating for years, “and it’s working. Patients are using it. Providers are using it. It’s well received.” Hopefully, she said, Congress will realize that “while they’ve given the authority to grant access to telehealth, it could go away if they don’t act.”
订阅 GLG 洞见趋势月度专栏
输入您的电子邮件,接收我们的月度通讯,获取来自全球约 100 万名 GLG 专家团成员的专业洞见。
